Singapore has one of the highest rates of diabetes in the world. There are many long term complications associated with diabetes and gum disease is one of them.
The relationship between diabetes and gum disease (periodontitis) is bi-directional. This means that not only are diabetic patients more prone to periodontitis, but periodontitis can also make it more difficult for diabetics to control their blood sugar level. In the United States, it has been shown that diabetic patients are up to 4.2 times more likely to develop periodontitis than those without diabetes.
What is periodontitis?
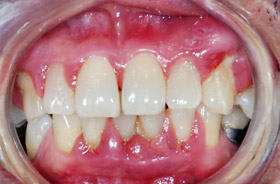
38 year old patient with periodontitis
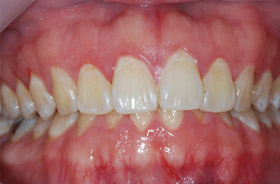
27 year old patient with gingivitis
Periodontal disease, more commonly called gum disease, is a long-standing bacterial infection of the gums. It is caused by plaque, which is a sticky, colourless or slightly yellow layer that forms on teeth throughout the day. In the early stage of the gum disease called gingivitis, the bacteria in plaque produces toxins (poisons) that leads to red and swollen gums. Sometimes though, the gums do not appear red but normal looking. As the disease progresses to periodontitis, the toxins destroy the bone supporting the teeth. Although there is little pain in the early stages of periodontitis, gum swellings, pain and loosening of teeth may develop later.
Diabetes – How does having diabetes affect my gums?
In diabetic patients, the white blood cells (which protect against infection) are defective. The amount of collagen necessary for healthy gums and good healing capacity are also reduced. This is worse in poorly-controlled diabetics. Hence, poorly-controlled diabetics have a poor healing capacity and an increased risk to periodontitis. Periodontitis is also more severe in diabetics with more advanced diabetic complications and in those who have had diabetes for a longer time.
Well- controlled diabetics have a lesser risk to periodontitis compared to poorly-controlled diabetics.
How does diabetes affect the rest of the mouth?
Those with uncontrolled or poor-controlled diabetics may experience a burning sensation in the mouth or tongue due to a reduced flow of saliva. There may also be an increased risk to tooth decay and fungal infections.
How is periodontitis treated in a diabetic patient?
The Periodontist (dental surgeon who specializes in gum disease) needs a certain amount of medical information such as the patient’s blood sugar level and the type of medication he/she is on. Treatment may need to be modified according to the medication the patient is on and how well the diabetes is controlled.
A well-controlled diabetic is usually treated similar to a non-diabetic with periodontal disease unless there are other medical conditions present. Patients are instructed to take their medications as prescribed and eat a normal breakfast. Early morning appointments are preferred as a certain type of hormone that reduces stress is in greater quantities in the morning.
A poorly-controlled diabetic will be treated in collaboration with his/her doctor or endocrinologist. Gum treatment is still encouraged though these patients may not respond the same as well –controlled diabetics. Some studies in the United States suggest that controlling periodontitis in the poorly-controlled diabetics may contribute to better blood sugar control.
In general, gum treatment consists of multiple sessions of deep scaling beneath the gums usually with local anaesthetic. In certain cases, surgical treatment may be recommended. Periodontal treatment may also be combined with treatment from other dental specialities if replacement of lost teeth is required.
Osteoporosis – How does osteoporosis affect my gums?
At the present moment, there is a weak association between osteoporosis and gum disease. This means that we are still unsure how osteoporosis can affect the amount of bone loss that occurs in periodontitis (gum disease) but there seems to be a link. Gum disease does not cause osteoporosis. Past studies suggest that osteoporosis may lead to tooth loss because the density of the bone that supports the teeth may be decreased and that hormone replacement therapy may offer some protection. More research is currently being done in this area to decipher and prove this link.
What is more important is the medication that is used to treat osteoporosis. One of the more commonly used medication nowadays is Fosamax. Fosamax belongs to a category of medications called bisphosphonates.
For those patients on Fosamax or a similar medication, there is a small risk of contracting osteonecrosis (destruction of the jaw bone) whenever an extraction or oral surgery has to be done. However, this risk increases after 3 years of continuous usage.
This means that patients on Fosamax should have regular dental checks and maintenance to prevent the need of ever having to undergo an extraction or surgery for the rest of their lives.
Patients are also usually sent by their doctors before the commencement of this type of medication for a dental clearance. Hence, it is always good to make sure we have healthy gums and teeth at any point of your lives as we can never know, especially for women, when osteoporosis will occur. Once a patient needs the medication and dental clearance is required, often there is insufficient time for the Periodontist (gum specialist) to get the gum disease under control. As such, if the periodontitis cannot be brought under control and yet the patient needs the medication, often extractions are carried out. We can avoid losing teeth in this manner if we get our gums checked at regular intervals. Losing teeth as we grow older is a myth!
What should I do to keep my oral health optimal at all times?
Prevention is always best.
Optimal oral health can be achieved via:
- A. Good control of diabetes via medication, diet, exercise as advised by the doctor
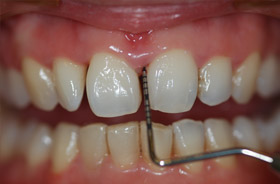
- B. Regular dental check ups that include gum checks and X-rays. Gum checks are done with a periodontal probe that takes measurements in the gum crevices
- C. Regular scalings or periodontal maintenance by a dentist or periodontist
- D. Regular scalings or periodontal maintenance by a dentist or periodontist